Every health plan needs a GLP-1 strategy in 2024. Between the off-label usage of Ozempic® and Mounjaro® to the emergence of the weight-loss-only versions, Wegovy® and Zepbound®, every employer from small to jumbo is debating what to do for these drugs.
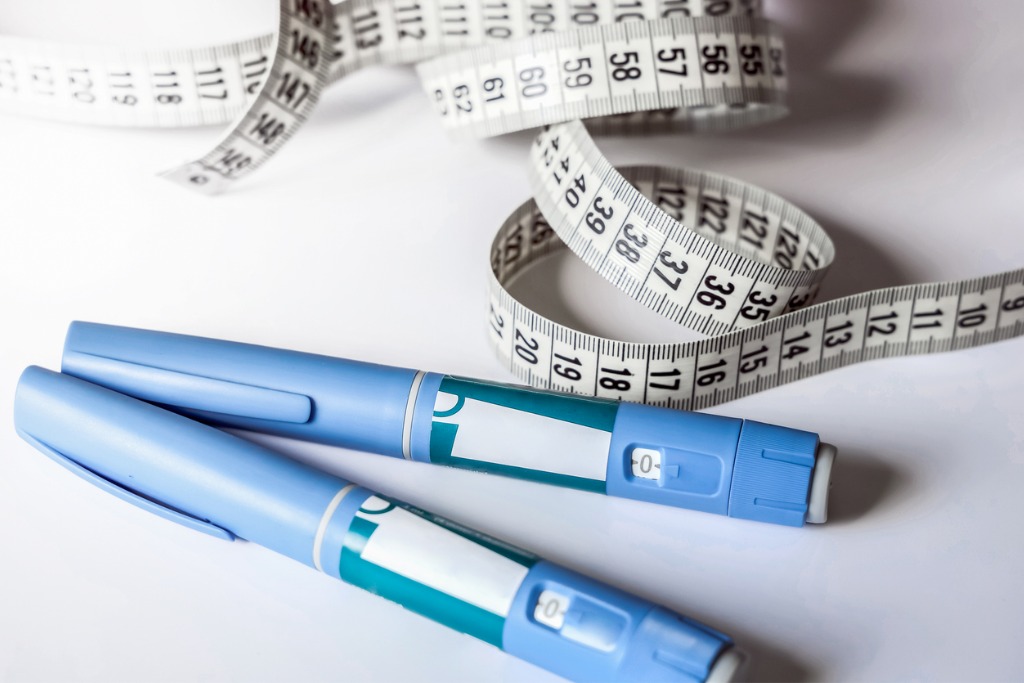
What’s Happening?
According to IQVIA, the use of Ozemipc, a popular GLP-1, is increasing by 75% over a rolling 12-month average.1 With a total of five GLP-1 medications on the market, a plan without a strategy to control the cost and usage of these medications risks astronomical price and premium increases. A recent study by the company Found, an online weight loss provider, indicated that 69% of participants did not have insurance coverage for GLP-1 medications which is a significant decrease over the past seven months.2
The first move in this chess game has been defensive – employers are removing coverage for GLP-1 medications for weight loss indications to avoid the cost impact on the plan. Some self-funded employers were not given a chance, finding out during renewal their ASO carrier decided to start covering the weight-loss-only GLP-1s. These employers are now faced with the difficult decision of whether to continue to provide coverage or stop with patients already on treatment plans with these meds. In addition, only deploying defensive strategies may put more pressure on HR departments from members who continue to hear about the benefits of these meds promoted by celebrities and pharmaceutical companies.
Additionally, preventing access to these drugs may have second-order implications further down the road from an unmanaged care perspective.
Cost to Health Plans if Weight Loss Drugs are Covered?
With the average cost of these medications around $1,000 per patient per month, the cost to cover these medications can be quite large, with an obesity rate of about 40% in the U.S. If you assume even a small portion of eligible patients on a plan utilize these medications, that is a substantial increase in drug cost in an environment where premiums are already rising year over year, and medication costs are exceeding the rate of inflation.
What are the Available Strategies?
Opt-out or Limit Coverage:
Plans can consider limiting GLP-1 medications for diabetic patients or excluding coverage. Plans need to consider that removing coverage for all GLP-1 medications may prevent patients with diabetes from access. Plans should be requesting PBMs provide criteria for coverage when limiting to diabetes and hire a third-party auditor to ensure criteria are being followed. This strategy includes the lowest risk of unmanaged cost but will need to continually be evaluated as the medications are indicated for use for other conditions such as cardiology, addiction, etc. In addition, not covering these medications at all may not be a feasible option for larger employers.
Require Participation in a Lifestyle Program:
Similar to bariatric surgery and certain transplant approval criteria requiring patients to change unhealthy behaviors, some employers are looking at requiring members to participate in a lifestyle or health coaching program prior to or in conjunction with covering these medications. This strategy may select patients committed to long-term behavior changes to prevent weight gain if or when these drugs are stopped. This program may cause some friction for both participants and providers as it can be seen as a delay tactic if there is a required participation period before drug approval.
Controlled Med Cost
When employers decide to cover GLP-1 weight loss medications, there are options to mitigate the full cost impact of these drugs, and the plan sponsor may be able to satisfy all stakeholders.
Personal importation, rebates, custom cost sharing, utilizing manufacturer copay assistance, and medication assistance programs are a few options historically used to mitigate drug costs, but the methods weren’t universally applicable or acceptable to all members. Now there is a way to leverage 340b pricing for these medications and capitate the medication cost for all members.
MakoRx Integrated Health Management (IHM) program is a new and innovative option that leverages 340b pricing to provide significant cost-savings for these medications. MakoRx provides GLP-1 medications to employer groups at an average 50% discount and the best part is patients have $0 cost for their medications. This program not only covers GLP-1s but all related branded diabetes medications and testing supplies. As one of the top areas of cost for any plan, having a strategy to control and capitate the cost of diabetes and obesity, that includes all the GLP-1 medications is the ideal solution for any employer group. If an employer wants to add this cost containment program on top of a lifestyle change solution, they may have optimal success and cost containment in one singular strategy.
How Does it Work?
MakoRx’s IHM strategy is a carve-out that can be implemented at any time for your plans, and there is no need to change the existing plan structure. All qualifying diabetic or weight loss patients are identified and transitioned to the program, which includes oversight by a clinical pharmacist and an additional virtual provider who coordinates with the patient and their existing care team. There is continuity of care, and additional providers provide a higher touch for the patient to improve adherence and positive trends in disease management for additional savings for the plan.
Why Isn’t Everyone Doing This?
MakoRx’s IHM program is premised on the ability to utilize highly discounted 340b pricing on these medications to pass through the savings to the patients and the plan. Because the ability to provide 340b pricing is tied to a provider network, there are very few 340b contract holders with a national provider network able to support a plan’s employees wherever they reside. In addition, telehealth regulations require the provider to be licensed in the state where the patient resides, so historically, this program and its associated deeply discounted pharma pricing have not been able to be utilized for employer plans.
Further complicating the matter is a traditional PBM’s incentive to profit off brand rebates for these meds. Increasing usage means increasing rebates, and a PBM that doesn’t fully pass rebates through will see this as a profit center.
Who Can Use this Program?
The beauty of IHM through MakoRx is that anyone can use this program, and you don’t have to wait for a new plan year to start. This tool will help you provide substantial value to your existing clients and also provide you with a valuable tool to win new business by showing a willingness to employ innovative solutions that shift the value from the PBM to the plan and the patient.
Want to Learn More or Have a Deeper Conversation About GLP-1s?
Contact MakoRx today to learn more.
References
- IQVIA, National Sales Perspectives, 2023
- GLP-1 drugs are still in demand. Insurers are cutting back coverage in response, Found study shows. Paige Minemyer Jul 26, 2023